-
Address:
17888 67th Court North
Loxahatchee, FL
-
Mail us:
contact@wrightacademia.org
- submit manuscript
Journal of Surgery and Clinical Reports
Table of content
Case Report |
Open Access |
Volume 1 | Issue 1 |
Necrotizing Soft Tissue Infection by Aspergillus in the Breast and Gluteal Region: Case Report
Fatih Doğan, MD* and Fatma Nilay Tutak, MD
Department of Plastic, Reconstructive and Aesthetic Surgery, Faculty of Medicine, Adıyaman University, Turkey
*Corresponding author: Fatih Doğan, MD, Department of Plastic and Reconstructive Surgery, Faculty of Medicine, Adıyaman University, 02200, Turgut Reis, Adıyaman, Turkey, Tel: +904162232320, Fax: +904162145599, E-mail: fatihdogan.prec@gmail.com
Citation: Doğan F, Tutak FN (2021) Necrotizing Soft Tissue Infection by Aspergillus in the Breast and Gluteal Region: Case Report. J Surg Clin Rpts 1:007.
Copyright © Doğan F, et al.
Received: |
Accepted: |
Published: |
Aspergillus infection of soft tissue is rare and typically affects immune compromised patients in several different patterns of clinical presentation. However, cutaneous aspergillosis can occur in both immune competent and immune compromised individuals due to trauma, surgery, or burn injury, or by direct inoculation of the fungus at the injury site. Skin involvement may result from direct inoculation of the fungus as well as from microemboli in disseminated aspergillosis. Here, we present a case with simultaneous necrotizing soft tissue infection of the breast and hip due to invasive aspergillosis.
Introduction
Necrotizing soft tissue infections are a broad category of bacterial and fungal skin infections. Descriptive terms vary based on the location, depth, and extent of infection (e.g., Fournier's gangrene [necrotizing perineal infection], necrotizing fasciitis [deep subcutaneous infection]). Depending on the depth of invasion, necrotizing soft tissue infections can cause extensive local tissue destruction, tissue necrosis, systemic toxicity, and even death. Although necrotizing soft tissue infections can be monomicrobial, they usually are synergistic polymicrobial infections. Non-clostridial necrotizing soft tissue infections are often polymicrobial, with more than 90% caused by beta-hemolytic streptococci or coagulase-positive staphylococci, and the remaining 10% associated with gram-negative enteric pathogens [1,2].
Necrotizing soft tissue infection caused by Aspergillus spp. (cutaneous aspergillosis) is an uncommon manifestation of aspergillosis. The prevalence of cutaneous aspergillosis is not exactly known, although necrotizing soft tissue infections involving aspergillus are very rare. Cutaneous aspergillosis can occur in both immune competent and immunodeficient individuals, due to trauma, surgery or burn injury, or through the direct inoculation of the fungus at the injury site [3]. Skin involvement may result from microemboli in disseminated aspergillosis, as well as from the direct inoculation of the fungus [4]. We present here a case with simultaneous necrotizing soft tissue infection of the breast and hip due to invasive aspergillosis.
Case Report
The 94-year-old female patient had no comorbidities other than chronic obstructive pulmonary disease and diabetes, regulated with oral anti-diabetic agents. While undergoing ampric antibio therapy for pulmonary infection in the hospital, the patient's condition deteriorated and she developed chest pain. The patient was consulted by a cardiologist, and by us when redness and pain developed in the breast tissue. The patient's breast ultrasound revealed no abscess, although edema was identified in all layers, which suggested cellulitis. No growth was observed in blood cultures, and a complete blood count showed progressively increased WBC (white blood cell) with neutrophil predominance. Body temperature measurements of the patient were normal. Upon observing the transformation of the red site on the breast into skin necrosis after 12 hours, the patient was taken for surgery, and a debridement of the site on the breast and tissue sampling were performed (Figure1A, Figure 1B and Figure 1C). Simultaneous with the lesion on the breast, necrosis occurred in the gluteal region of the patient (Figure 1E and Figure 1F). The tissue samples sent to pathology revealed Aspergillus (Figure 2). Despite 5 days of serial debridement and wound care, the necrosis site continued to increase in size, and there was a marked white hypha-like presentation accompanied by dry necrosis (Figure 1D). Aggressive surgical debridement and intravenous antifungal therapy continued, however the patient's condition deteriorated clinically, resulting in death.
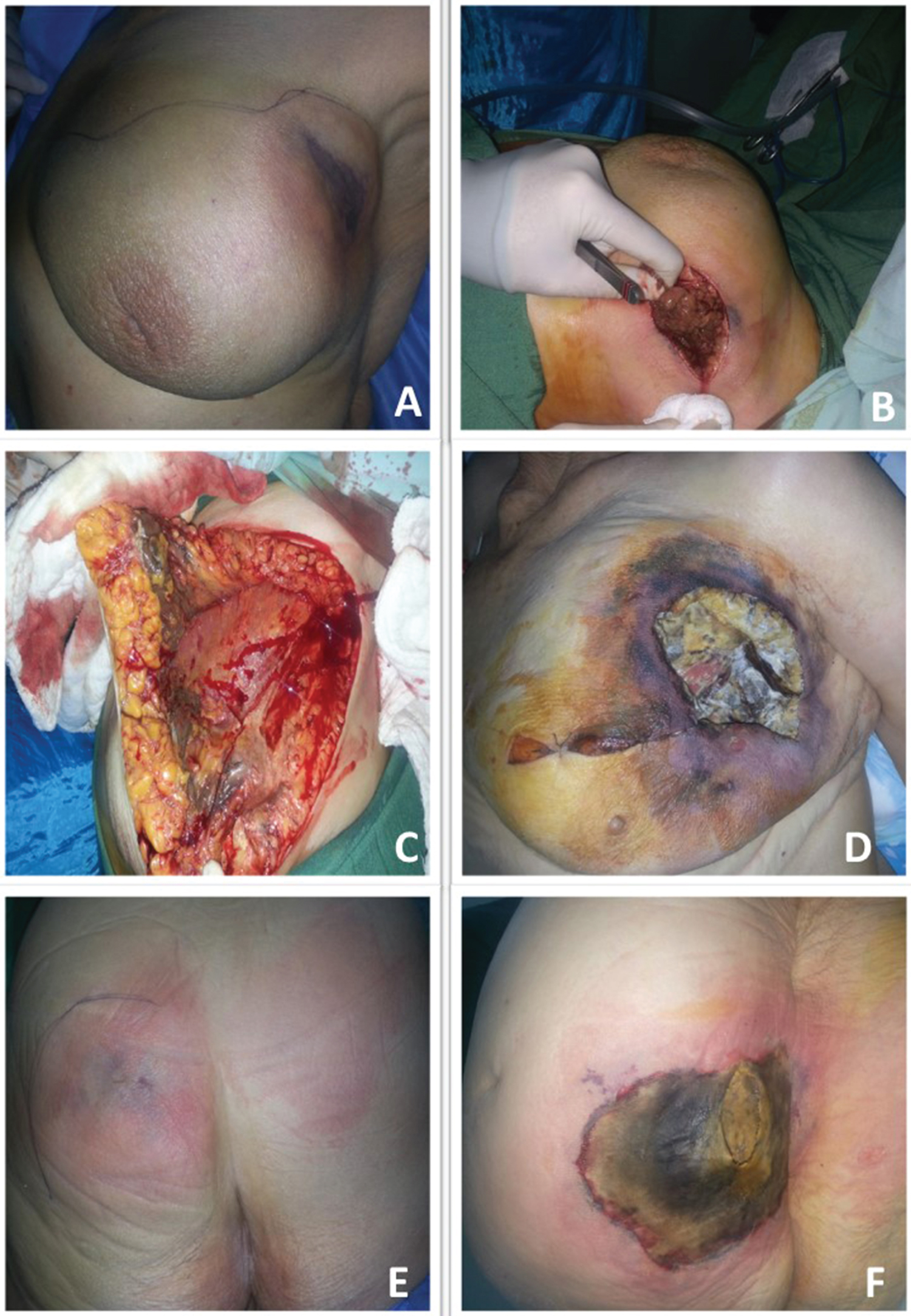
Figure 1: (A) Onset of the lesion in the upper outer quadrant of the left breast; (B) Debridement of the lesion in the breast; (C) Intraoperative view of the necrosis site; (D) The surgical site after 24 h of debridement; (E) Simultaneous onset of a lesion in the hip; (F) Day 3 view of the lesion on the hip.
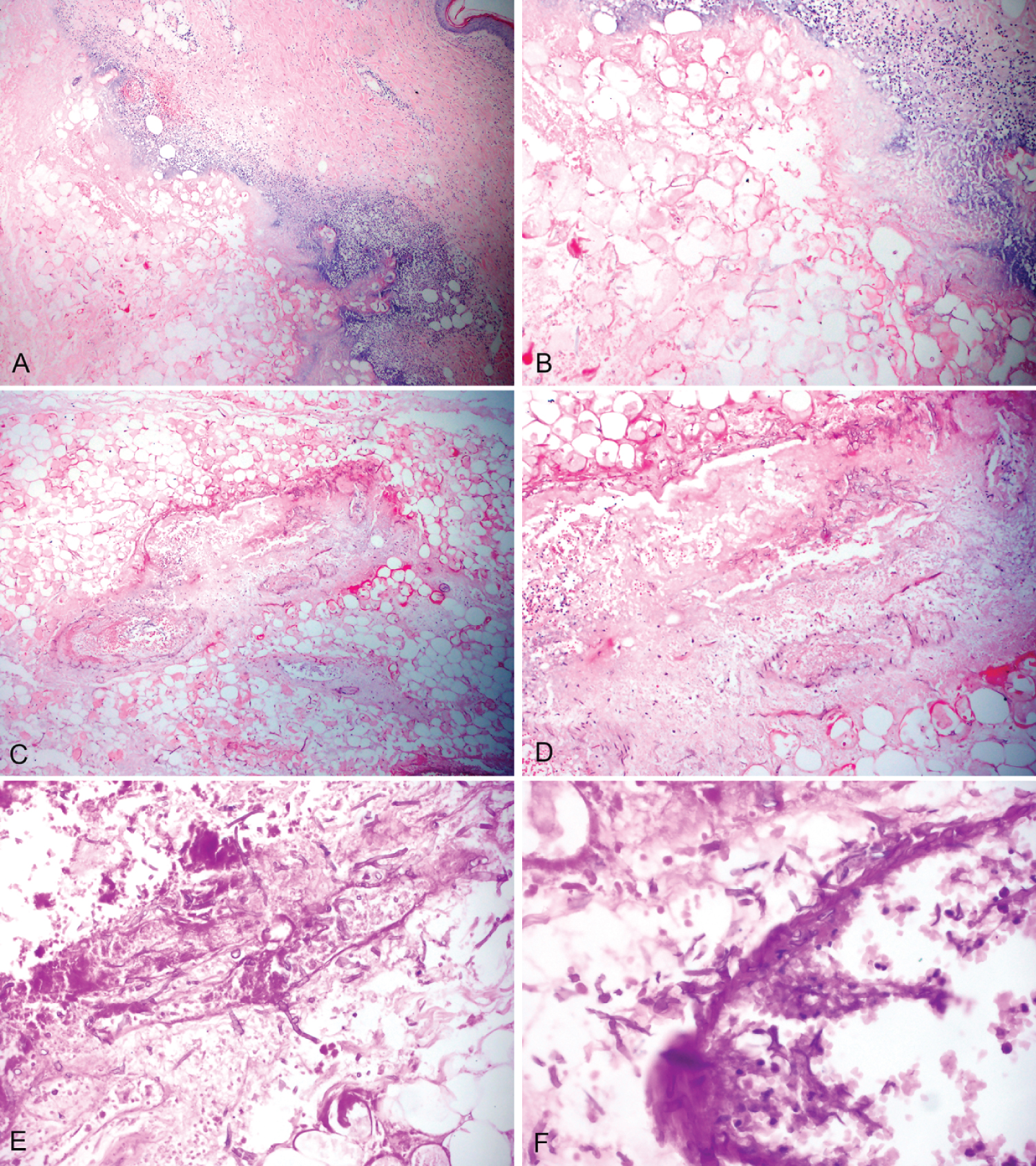
Figure 2: (A,B) Necrosis and inflammation starting in the deep dermis and progressing to adipose tissue. (Hematoxylin-Eosin, x40 and x100); (C,D) There was marked necrosis on the vessel walls besides fat necrosis, and there were remarkable fungal hyphae both in the adipose tissue and on the vessel walls. (Hematoxylin-Eosin, x100 and x200); (E,F) Branching hyphae to be consistent with Aspergillus spp. (PAS x100 and x200).
Discussion
Invasive aspergillosis - an opportunistic infection - may lead to pulmonary infection in patients with hematological malignancies, and especially those with prolonged neutropenia, solid organ tumors, intensive care stay, HIV and those undergoing allogeneic stem cell and solid organ transplantations. The patients in all these groups are immunodeficient, to a certain extent. Extra pulmuner involvement forms of aspergilliosis reported in the literature have been reported as aspergillosis rhinosinusitis, ocular aspergillosis, aspergillus osteomyelitis and central nervous system aspergillosis [5]. Sinus aspergillosis may present as a fungus ball of the sinus cavity, allergic sinusitis, granulomatous rhinosinusitis, or as invasive sinus disease. Invasive fungal sinusitis can be acute with a fulminant and rapid clinical course, such as in the immune suppressed population or, less commonly, in patients without identifiable immune defects, as a chronic granulomatous form with progression through the sinus mucosa, underlying tissue, and bone. This latter form is seen primarily in the Middle East for reasons that are unclear but may relate to host immunogenetic factors [6]. Aspergillosis of the eye can present as dacryocystitis, periorbital cellulitis, endophthalmitis, vitritis, or may be secondary to contiguous extension from invasive sinusitis or dissemination from a primary pulmonary site. Keratitis also is a common ocular manifestation following local exposure [5]. An osteomyelitis is a rare entity. It is most often seen in patients with significant immune suppression, including chronic granulomatous disease, hematological malignancies, solid organ transplantation, HIV infection, steroid therapy, or prior or concurrent pulmonary aspergillosis. Infections following penetrating trauma or as a complication of recent surgery or procedure have also been reported [7]. Central nervous system aspergillosis usually occurs in patients with neutropenia. Cerebrospinal fluid analysis is not typically useful for diagnosis because most central nervous system aspergillosis manifests as a mass lesion instead of meningitis [5].
Skin involvement is very rare, with only a few cases presented as case studies in literature to date. To the best of our knowledge, there has been no case in literature reporting on the sudden development of lesions in two independent foci in the body presenting with aggressively necrotizing soft tissue infection in a patient without immunodeficiency, as was the case with our patient. The progressively increasing white blood cells with neutrophil predominance in a complete blood count indicates a severe immune reaction, while the subcutaneous onset in two separate anatomical locations leading to soft tissue necrosis suggests it to be caused by microemboli due to disseminated aspergillosis. It was our wish to highlight here that such a sudden primary lesion in the breast tissue may be attributable to aspergillosis.
Ethical Statement
The authors did not receive support from any organization for the submitted work. All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest or non-financial interest in the subject matter or materials discussed in this manuscript. The patient was informed about the procedures. Informed consent form was obtained from the patients and their relatives.
Declarations
Funding
There is no financial support related to this manuscript.
Competing interests
Both authors declare that they have no competing interests.
Authors' contributions
FD made substantial contributions to operation and writing, FNT made substantial contributions to data interpretation and writing. Both authors read and approved the final manuscript.
Acknowledgements
The patient was informed about the procedures. Informed consent form was obtained from the patients and their relatives.
References
- Johnson MA, Lyle G, Hanly M, et al. (1998) Aspergillus: A rare primary organism in soft-tissue infections. Am Surg 64: 122-126.
- Elliott D, Kufera JA, Myers RA (2000) The microbiology of necrotizing soft tissue infections. Am J Surg 179: 361-366.
- Marcus JR, Palella FJ, Yeldandi AV, et al. (1999) Extent of surgical intervention in primary soft-tissue aspergillosis. Ann Plast Surg 42: 683-687.
- Denning DW, Stevens DA (1990) Antifungal and surgical treatment of invasive aspergillosis: Review of 2,121 published cases. Rev Infect Dis 12: 1147-1201.
- Cadena J, Thompson GR 3rd, Patterson TF (2016) Invasive Aspergillosis: Current Strategies for Diagnosis and Management. Infect Dis Clin North Am 30: 125-142.
- Thompson GR 3rd, Patterson TF (2012) Fungal disease of the nose and paranasal sinuses. J Allergy Clin Immunol 129: 321-326.
- Gabrielli E, Fothergill AW, Brescini L, et al. (2014) Osteomyelitis caused by Aspergillus species: A review of 310 reported cases. Clin Microbiol Infect 20: 559-565.
INDEXING
PARTNERS








